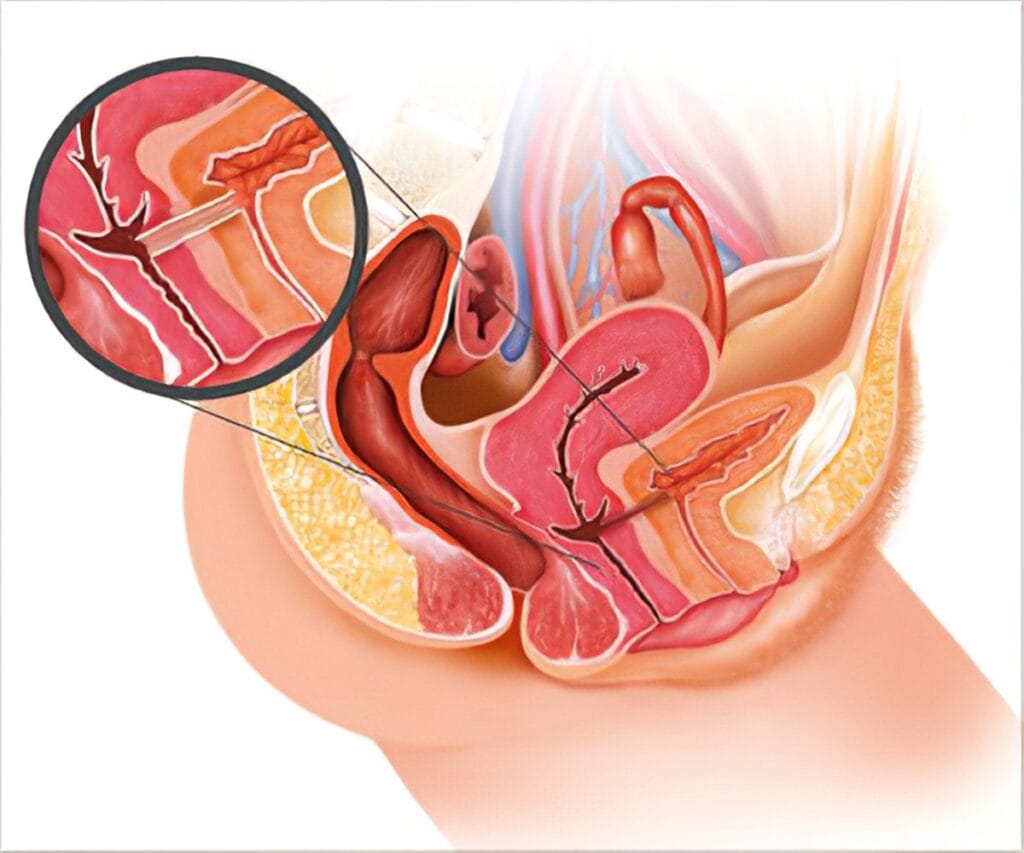
Vesicovaginal fistula (VVF) is a severe medical condition characterized by an abnormal connection between the bladder and the vagina, leading to continuous, uncontrollable leakage of urine and sometimes faeces. This condition is debilitating and predominantly affects women in low-resource settings, often as a result of prolonged and obstructed labour. Without timely medical intervention, VVF can cause significant physical and psychological distress, social ostracization, and a profound decrease in the quality of life. Vesico-Vaginal Fistula (VVF), as seen in Nigeria, is a major cause of severe morbidity and potential mortality, which can result in marital disruption, rejection and eventual destitution.
Other causes include “gishiri cut,” cervical carcinoma, surgical trauma such as caesarean section, hysterectomies, infection and other gynaecological procedures. Traditional practices such as female genital mutilation and long episiotomies popularly known as gishiri cuts in northern Nigeria. Women with VVF often face stigma and depression and may be ostracized from their communities due to the smell of urine. They are also typically poor, illiterate women who live in rural areas with few means of earning a living.
According to one of the oldest and globally recognised medical journals, Lancet, vesicovaginal fistula (VVF) is “a serious medical disorder characterised by an abnormal opening between the vagina and the bladder or rectum, which results in continuous leakage of urine or stool.”
The exact magnitude of VVF worldwide is unknown. However, the World Health Organization (WHO) estimates that over 20 million women are living with this condition,
According to the United Nations Children’s Fund (UNICEF), between 400,000 and 800,000 Nigerian women are living with VVF and between 50,000 and 100,000 new cases are added every year. The United Nations agency said Nigeria has a prevalence of obstetric fistula, as VVF is also known, of 3.2 per 1000 births. It bemoans the slow rate of fistula repairs caused by inadequate fistula surgeons and the high rate of new cases. The agency estimated that it may take up to 83 years to clear the backlog of cases at the current rate of repair.
Symptoms of Vesico-Vaginal Fistula (VVF)
Vesico-Vaginal Fistula (VVF) occurs when there is an abnormal opening between the bladder and the vagina, leading to involuntary leakage of urine. The condition mainly affects women, especially in settings where access to proper maternal healthcare is limited. VVF is most commonly caused by prolonged obstructed labor but can also result from surgery, trauma, or infection.
Here are the key symptoms of VVF:
- Constant Leakage of Urine
The most common and prominent symptom of VVF is continuous, uncontrollable leakage of urine through the vagina. This occurs because the fistula allows urine to flow from the bladder into the vaginal canal.
- Involuntary Urination: Women with VVF may have no control over their urination, leading to continuous wetness.
- Odor: The leakage of urine can lead to a strong, persistent smell, contributing to social embarrassment and discomfort.
- Wetness in the Genital Area
Because of the constant urine leakage, women with VVF experience persistent wetness in the vaginal and genital areas. This can lead to skin irritation or infections due to constant moisture.
- Skin Maceration: Prolonged wetness can cause irritation, rashes, or sores in the skin surrounding the genital area.
- Infections: There is an increased risk of vaginal infections or urinary tract infections (UTIs) due to constant exposure to urine.
- Urinary Incontinence
VVF results in a total loss of control over urination, making it impossible for the affected woman to hold or control the flow of urine.
- Urge to Urinate: Some women may still feel the need to urinate, but they are unable to control the flow.
- Frequent Urination: Some may feel as though they need to urinate frequently, despite already leaking continuously.
- Recurrent Urinary Tract Infections (UTIs)
Due to the abnormal connection between the bladder and the vagina, women with VVF are at higher risk of developing recurrent UTIs. The mixing of urine and vaginal fluids creates an environment where bacteria can thrive.
- Symptoms of UTI: These can include painful urination (dysuria), frequent urination, and a burning sensation when urinating.
- Cloudy or Foul-Smelling Urine: Urine may have a strong odor or appear cloudy due to infection.
- Pain or Discomfort
While some women with VVF may not feel pain, others may experience discomfort or pain, particularly if infections develop or if the surrounding tissues are irritated by constant moisture.
- Pelvic Pain: Some women may experience lower abdominal or pelvic pain, especially if the fistula is associated with prolonged labor or surgical trauma.
- Vaginal Pain: Irritation or infections can cause discomfort in the vaginal area.
- Social and Psychological Symptoms
In addition to the physical symptoms, VVF often causes significant emotional and psychological distress due to the social consequences of the condition.
- Social Isolation: Many women with VVF are shunned by their communities or families due to the persistent smell of urine and incontinence, leading to isolation.
- Depression and Anxiety: The loss of control over bodily functions, combined with social stigma, can lead to depression, anxiety, and low self-esteem.
- Possible Co-Existing Symptoms (Related to Prolonged Labor)
In cases where VVF is caused by prolonged obstructed labor, other complications may accompany the fistula, including:
- Recto-Vaginal Fistula (RVF): This is when an abnormal opening forms between the rectum and vagina, causing fecal incontinence. Women with both VVF and RVF may leak both urine and feces through the vagina.
- Foot Drop or Nerve Damage: Prolonged labor can cause nerve damage, resulting in conditions like foot drop, where the woman cannot lift the front part of her foot.
- Pelvic Organ Prolapse: Prolonged or obstructed labor can cause pelvic organs (such as the bladder or uterus) to slip out of place, leading to further discomfort and dysfunction.
- Symptoms Related to Post-Surgical Fistulas
If VVF results from surgical trauma (such as after a hysterectomy or cesarean section), symptoms may appear shortly after surgery:
- Immediate Urine Leakage: Women may notice leakage of urine soon after surgery.
- Delayed Symptoms: In some cases, the symptoms may not appear immediately and can develop weeks or months after the surgery as the fistula gradually enlarges.
The hallmark symptom of VVF is continuous and involuntary urine leakage, often accompanied by skin irritation, recurrent infections, and significant emotional and social consequences. Early diagnosis and medical intervention are critical to address the physical and psychological impact of VVF and improve the quality of life for affected women.
Care and Management for VVF
The management and care of VVF involve a combination of medical, surgical, psychosocial, and community-based approaches. Here’s how VVF is typically cared for and managed:
- Preventive Care
Prevention plays a critical role in reducing the incidence of VVF, particularly in low-resource settings where access to maternal healthcare is limited. Key preventive strategies include:
- Access to Skilled Birth Attendants: Ensuring that women have access to trained health professionals during childbirth to manage complications like obstructed labor.
- Timely Access to Cesarean Section: Prompt surgical intervention, such as a cesarean section, can prevent the development of VVF by relieving prolonged obstructed labor.
- Antenatal Care: Regular prenatal visits to identify and manage high-risk pregnancies and promote maternal health.
- Education and Community Outreach: Educating communities about the importance of maternal health services and the risks of obstructed labor.
- Diagnosis of VVF
Accurate diagnosis of VVF is essential for proper treatment. Diagnosis involves:
- Medical History and Physical Examination: A detailed medical history, including any history of prolonged labor, surgery, or trauma, is essential. A pelvic examination is usually performed to detect any leakage of urine from the vagina.
- Diagnostic Tests:
- Dye Test: A common test where a dye is injected into the bladder, and any leakage from the vagina confirms the presence of a fistula.
- Cystoscopy: A procedure that uses a scope to view the inside of the bladder and locate the fistula.
- Imaging: In some cases, imaging techniques like ultrasound or MRI may be used to assess the extent of the injury.
- Surgical Management of VVF
Surgery is the main treatment for repairing VVF. The success rate of surgery is high, particularly when performed by skilled surgeons. Surgical interventions include:
- Fistula Repair Surgery
- Timing: Surgery is usually performed 3 to 6 months after the injury to allow any inflammation to subside, though early interventions can sometimes be done.
- Procedure: The surgeon closes the fistula by suturing the tissues between the bladder and vagina. In cases of large or complex fistulas, tissue grafts may be used.
- Types of Repairs: Fistula repairs can be performed through:
- Vaginal Route: The surgeon accesses the fistula through the vagina, which is the most common and preferred approach.
- Abdominal Route: For more complex or recurrent fistulas, an abdominal approach may be necessary.
- Post-Surgical Care: After surgery, patients are usually advised to have a catheter in place for 10 to 14 days to allow the tissues to heal. Proper catheter care and infection prevention are essential during this period.
- Surgical Success Rate
- Success Rates: For simple fistulas, the success rate is around 85-95% after the first surgery. For complex or recurrent fistulas, success rates can be lower, requiring additional interventions.
- Post-Operative Care
After VVF surgery, ongoing care is crucial to ensure healing and prevent recurrence or complications. This includes:
- 1. Catheter Management
- Patients are kept with a catheter in place for up to 14 days after surgery to divert urine away from the surgical site, allowing proper healing.
- Catheter Care: Patients are educated on how to manage their catheter to prevent infections or blockage. Cleanliness and hydration are important aspects of catheter care.
- Nutritional Support
- Proper nutrition is vital for post-surgical recovery. A balanced diet rich in proteins, vitamins, and minerals helps to promote tissue healing and overall recovery.
- Infection Prevention
- Antibiotics may be prescribed to prevent infections during the post-operative period. Regular follow-up visits help monitor healing and detect any signs of complications.
- Physical and Emotional Rest
- Women are advised to avoid heavy lifting or sexual intercourse for several months after surgery to prevent stress on the healing tissues.
- Long-Term Care and Follow-Up
Many women with VVF require long-term support even after successful surgical repair. This includes:
- 1. Physical Rehabilitation
- Pelvic Floor Exercises: These exercises help strengthen the pelvic muscles, which may have weakened due to prolonged labor or surgery.
- Bladder Training: For women who have experienced long-term incontinence, bladder training may be necessary to regain control over urinary function.
- 2. Psychosocial Support
- Counseling: Women who have suffered from VVF often experience severe social, emotional, and psychological distress. Counseling services help them cope with the trauma and rebuild their self-esteem.
- Support Groups: Joining support groups with other VVF survivors can provide emotional solidarity, shared experiences, and a sense of community.
- 3. Addressing Social Stigma
- Women with VVF often face stigma and isolation in their communities. Part of the long-term care involves community reintegration efforts, including educating the community to reduce stigma and raise awareness about VVF.
- Empowerment and Skills Acquisition
To aid full recovery and empowerment, many NGOs and healthcare organizations provide skills acquisition programs for VVF survivors. These include:
- Vocational Training: Programs in tailoring, agriculture, or small-scale entrepreneurship are common, helping survivors gain financial independence.
- Education and Reintegration: NGOs often provide literacy classes and advocacy to help survivors reintegrate into their communities and advocate for maternal health issues.
- Management of Complications
Although surgery is effective for most women, some may experience complications or recurrence. Management of these situations includes:
- Recurrence or Complex Fistulas
- Some women may develop recurrent fistulas, requiring additional surgeries or more complex interventions by specialist surgeons.
- Urinary Incontinence Post-Surgery
- Even after successful closure of the fistula, some women may continue to experience incontinence due to damaged bladder or urethral function. This is managed through:
- Physical Therapy: Pelvic floor exercises to improve bladder control.
- Medications: Certain medications can help manage bladder dysfunction.
- Secondary Surgery: In some cases, further surgical procedures are required to address incontinence.
- Community-Based Care and Advocacy
VVF care extends beyond medical treatment. Many organizations focus on advocacy, public awareness, and education to improve maternal health services and prevent VVF. Community-based care includes:
- Community Education: Educating women, families, and communities about maternal health, the risks of obstructed labor, and the importance of accessing skilled birth attendants.
- Improving Access to Maternal Health Services: NGOs work with local governments and international partners to improve access to obstetric care, including building healthcare facilities in rural areas and training healthcare workers.
The management and care of Vesico-Vaginal Fistula (VVF) require a comprehensive approach that includes preventive healthcare, skilled surgical intervention, post-operative care, psychosocial support, and community reintegration. With proper medical attention, VVF can be successfully treated, allowing women to regain their dignity, health, and independence. NGOs and healthcare organizations play a crucial role in providing these services and advocating for improved maternal health globally.
Recovery Time After Vesico-Vaginal Fistula (VVF) Surgery
The recovery process after VVF surgery varies depending on several factors, including the complexity of the fistula, the patient’s overall health, and the quality of post-operative care. On average, the recovery period spans several weeks to a few months. Here’s an overview of the key stages of recovery:
- Immediate Post-Surgical Recovery (1 to 2 Weeks)
Hospital Stay
- Duration: Most women stay in the hospital for 7 to 10 days after VVF surgery, though this may vary based on the healthcare setting and the complexity of the surgery.
- Catheter Use: A urinary catheter is usually placed during surgery and remains in place for 10 to 14 days to divert urine away from the healing tissues. The catheter ensures that the repaired fistula site is not exposed to pressure from urine flow.
Post-Surgical Monitoring
- Infection Prevention: Antibiotics may be administered to prevent infections, and pain management is provided to ensure patient comfort.
- Wound Healing: The medical team monitors the surgical site for signs of proper healing, checking for any complications such as infections or leakage of urine.
- Fluid Intake: Patients are encouraged to drink plenty of fluids to promote healing and maintain good kidney and bladder function.
- Home Recovery Phase (2 to 6 Weeks)
Once discharged, the patient continues the recovery process at home, focusing on healing, rest, and avoiding activities that might put stress on the surgical site.
Catheter Removal
- Timing: The catheter is typically removed after 10 to 14 days, depending on how well the surgical site has healed. In some cases, if healing is slower, the catheter may need to stay in place for a longer period.
- Monitoring for Leakage: After catheter removal, patients are observed to ensure there is no urinary leakage, which could indicate that the fistula has reopened or that there are other complications.
Physical Rest
- Rest: Patients are advised to avoid heavy lifting, strenuous activity, and sexual intercourse for at least 6 to 8 weeks after surgery to allow full healing of the repaired tissues.
- Movement: Gentle movement and walking are encouraged to maintain circulation and prevent complications such as blood clots, but any excessive physical strain should be avoided.
- Full Recovery (6 Weeks to 3 Months)
Healing Time
- For most women, complete healing from VVF surgery takes about 6 to 12 weeks. During this time, the tissues between the bladder and vagina continue to strengthen, and normal bladder function returns.
- Regular Check-Ups: Follow-up appointments are critical during this period to monitor healing and ensure there are no signs of infection, complications, or recurrence of the fistula.
Bladder Training and Pelvic Exercises
- Bladder Control: In some cases, women may experience temporary incontinence even after the fistula is closed, due to weakened pelvic floor muscles or bladder dysfunction. Bladder training or pelvic floor exercises can help improve control and restore normal urinary function.
Return to Normal Activities
- Light Activities: By 6 to 8 weeks post-surgery, most women can resume light activities and daily routines.
- Resuming Sexual Activity: Sexual intercourse should generally be avoided for at least 3 months post-surgery to prevent stress on the surgical site and ensure proper healing.
Nutritional Support
- A healthy diet rich in proteins, vitamins, and minerals helps promote tissue healing and overall recovery during this period. Staying hydrated is also crucial for maintaining good bladder health.
- Long-Term Recovery and Emotional Well-Being
In addition to physical recovery, many women face emotional and psychological challenges following VVF, particularly if they’ve experienced social isolation, stigma, or long-term incontinence before surgery.
Psychosocial Support
- Counseling: Emotional recovery may take longer and often requires counseling or psychosocial support to help women rebuild confidence and reintegrate into their communities.
- Support Groups: Many women benefit from joining support groups with other VVF survivors, which can help reduce feelings of isolation and provide a space to share experiences.
Reintegration into the Community
- For women who have been ostracized or isolated due to the stigma of VVF, community reintegration can be a gradual process. Programs that offer skills training and economic empowerment are important for long-term recovery and independence.
- Possible Complications During Recovery
While most women recover well from VVF surgery, some may experience complications that prolong the recovery process. These can include:
- Recurrence of the Fistula
- In about 10 to 15% of cases, especially with complex or large fistulas, the fistula may reopen, requiring additional surgery.
- Incontinence
- Some women may continue to experience urinary incontinence even after successful fistula repair due to bladder damage or weakness in the pelvic floor muscles. This can be managed through pelvic exercises, medications, or further surgical interventions.
- Infection
- Infection of the surgical site or urinary tract infections (UTIs) are potential complications. Proper catheter care, hygiene, and follow-up with healthcare providers are crucial to managing and preventing infections.
- Factors That Affect Recovery Time
Several factors can influence the length and success of recovery, including:
- Complexity of the Fistula: Simple fistulas tend to heal more quickly, while more complex or recurrent fistulas may require a longer recovery period.
- Overall Health: Women in good health generally recover more quickly, while those with other health issues (e.g., malnutrition, infection, or underlying medical conditions) may take longer to heal.
- Quality of Surgical Care: Access to skilled surgeons and high-quality medical care greatly affects the success of surgery and the speed of recovery.
- Support System: Emotional and social support from family, healthcare providers, and community organizations can positively influence a woman’s recovery process.
The typical recovery time after VVF surgery is around 6 to 12 weeks, with most women resuming normal activities within this timeframe. However, full recovery, including emotional and psychological healing, may take several months. Proper post-operative care, rest, follow-up visits, and psychosocial support are essential components of a successful recovery. With the right care and support, most women are able to regain their health, dignity, and independence following VVF surgery.
Can VVF be prevented?
Yes, Vesico-Vaginal Fistula (VVF) can be largely prevented through a combination of proper maternal healthcare, community education, and addressing the underlying social factors that contribute to the condition. Prevention efforts focus on reducing the risk factors that lead to VVF, particularly prolonged obstructed labor, which is the most common cause in low-resource settings.
Key Strategies for Preventing VVF:
- Access to Skilled Birth Attendants
- Skilled care during childbirth is one of the most effective ways to prevent VVF. Skilled birth attendants (such as midwives, doctors, or trained nurses) can monitor labor progress and manage complications before they result in fistulas.
- Early Identification of Obstructed Labor: With proper monitoring, skilled birth attendants can detect signs of obstructed labor early and take necessary actions, such as performing a cesarean section if required, to prevent the prolonged pressure on the bladder that leads to VVF.
- Timely Access to Emergency Obstetric Care
- Prolonged labor is the main cause of VVF, but it can be prevented with timely access to emergency obstetric care, including cesarean sections when labor becomes obstructed.
- Well-Equipped Health Facilities: Health centers must be equipped to provide emergency care, such as cesarean sections, blood transfusions, and other interventions that may be necessary during childbirth.
- Transportation and Referral Systems: In many rural or underserved areas, delays in reaching healthcare facilities are a major barrier. Ensuring that women can access emergency care quickly, through improved transportation and referral networks, can significantly reduce the risk of VVF.
- Antenatal (Prenatal) Care
- Regular prenatal check-ups are important to identify high-risk pregnancies that may result in obstructed labor or other complications. Early interventions can then be planned to avoid prolonged labor.
- Monitoring of Fetal Position and Maternal Health: During antenatal care, healthcare providers can monitor the baby’s size, position, and the mother’s health to determine if she might face difficulties during labor, making it possible to plan for a safe delivery.
- Family Planning and Birth Spacing
- Family planning can help prevent VVF by reducing the risk of prolonged or complicated labor in cases of early pregnancies, closely spaced births, or pregnancies in older women.
- Teenage Pregnancy Prevention: Young girls whose bodies are not yet fully developed for childbirth are at higher risk for obstructed labor and VVF. Providing access to contraception and education can help delay pregnancies until the woman’s body is mature enough for childbirth.
- 5. Education and Empowerment of Women
- Education plays a critical role in preventing VVF. Women who are educated are more likely to seek healthcare services during pregnancy and childbirth, understand the risks of home deliveries, and make informed decisions about their reproductive health.
- Empowerment of Women: Empowering women socially and economically enables them to have more control over decisions related to their health, including seeking timely medical care during pregnancy and childbirth.
- Reducing Early and Forced Marriages
- Early marriage is a significant risk factor for VVF, as girls who marry and become pregnant at a young age are more likely to experience complications during childbirth, including obstructed labor. Preventing early marriages through legislation, education, and advocacy can help reduce the incidence of VVF.
- Community Education and Outreach
- Educating communities about the dangers of prolonged labor and the importance of skilled care during childbirth can help prevent VVF. In many rural areas, women often give birth at home or with traditional birth attendants who may not have the skills to manage obstructed labor.
- Changing Social Norms: Community education programs can challenge traditional practices that may contribute to obstructed labor, such as encouraging home births without skilled attendants or delaying seeking help in an emergency.
- Nutritional Support and Maternal Health
- Malnutrition is a significant risk factor for VVF, as undernourished women are more likely to have stunted growth, narrow pelvises, and other conditions that increase the risk of obstructed labor.
- Improved Nutrition for Pregnant Women: Ensuring that women receive proper nutrition during pregnancy can improve maternal health and reduce the risk of complications during childbirth. This is particularly important for adolescent girls, whose bodies are still developing.
- Strengthening Healthcare Infrastructure
- Improving the overall healthcare system and infrastructure in low-resource settings can reduce the occurrence of VVF. This includes building more health facilities, ensuring that they are adequately staffed with trained personnel, and providing necessary medical supplies and equipment.
- Training of Healthcare Workers: Ensuring that doctors, midwives, and nurses are trained in safe delivery practices and the management of complications is crucial in preventing obstetric fistulas.
- Addressing Gender Inequality
- Gender inequality is a root cause of many maternal health issues, including VVF. In many parts of the world, women’s health is not prioritized, leading to delayed or denied access to care during childbirth.
- Advocacy and Policy Changes: Advocating for women’s rights, better maternal healthcare policies, and investment in maternal health services can help prevent conditions like VVF
- Timely Surgical Care for Other Causes of VVF
- In addition to obstructed labor, VVF can also be caused by surgical trauma (e.g., from a hysterectomy or cesarean section). Proper training of surgeons and healthcare providers in preventing and managing complications from these procedures can reduce the risk of post-surgical VVF.
Conclusion
VVF is a preventable condition with the right combination of education, access to healthcare, skilled birth attendance, and community support. By addressing the underlying causes—such as obstructed labor, early marriage, malnutrition, and lack of access to emergency obstetric care—VVF can be significantly reduced. Prevention efforts require collaboration between governments, healthcare providers, NGOs, and communities to ensure that women receive the care and support they need during pregnancy and childbirth.